by Dr. Allen Peabody
Now that school is back in session, knowledge, friendship, and pencils are not the only things that students will share. Unfortunately the end of summer also marks the beginning of the sick season with numerous infections easily spread from close contact. Strep throat is one of those common infections that results in a significant disease burden each year, and this is a fitting time to review it as well as its symptoms, how to diagnose it, usual treatment, and some potential complications.
Group A Strep
There are numerous species of streptococcus that cause various infections. When we say “strep throat”, we are actually referring to a specific species of Group A strep known as Streptococcus pyogenes. It is most commonly spread by close contact with someone who is infected through secretions from the nose or mouth. It can take 3-7 days to show symptoms once exposure has taken place. It is very common in the winter months and, at its peak, is estimated to be the cause of 30-35% of all sore throat illnesses.
Symptoms
The most common symptoms for school aged children are sore throat, fever, headache, vomiting, and tender lymph nodes in the neck. Looking in the throat can sometimes show large tonsils with exudates (white patches) and/or redness. Less commonly strep throat can cause a rough sandpapery rash known as “scarlett fever”. Children <5 usually have atypical signs and symptoms like low grade fevers, prolonged runny nose, vomiting, etc. that may be confused with another illness. Usually these younger children are exposed by their older siblings who are attending school. Most of the time there is decreased oral intake due to the pain/swelling in the throat.
Diagnosis and treatment
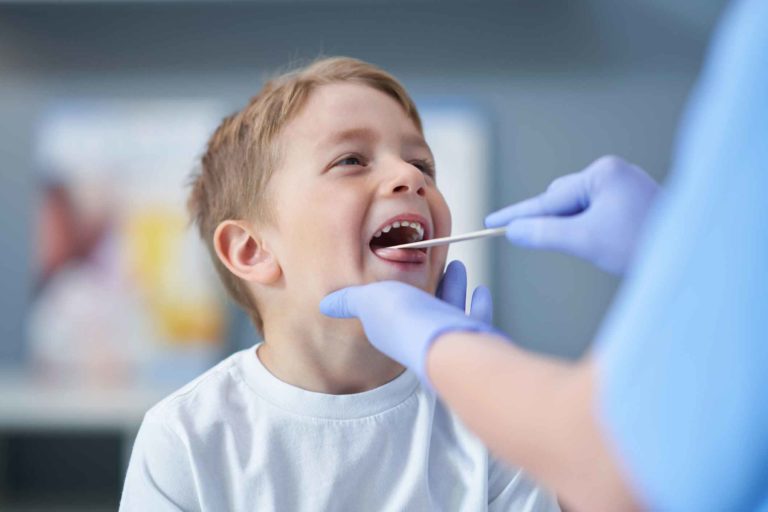
Strep throat must be diagnosed at a doctor’s office with a throat swab. Almost all offices use a rapid strep test that will give accurate results within 5-10 minutes. These tests are highly accurate if a positive result is obtained, but are less accurate for negative results. The standard of care is to culture negative rapid strep results to ensure that there is no strep infection which will take up to 48 hours to result.
Treatment of streptococcal sore throat is usually with oral antibiotics, most often with a penicillin based medicine or an alternative if there are allergies to penicillin. Occasionally the symptoms are so severe (unable to keep anything down, sever pain, etc.) that an intramuscular injection of antibiotics are given. The symptoms resolve rapidly and in most cases there is dramatic improvement within 24 hours. Students may return to school after they are both on antibiotics and fever free for 24 hours.
Potential complications
Group A strep can cause significant complications including neighboring spread of the bacteria causing abscess formations in the throat/tonsils, ear infections, or sinusitis. In addition it can also cause acute rheumatic fever, poststreptococcal glomerulonephritis (involvement in the kidneys) and exacerbation of OCD or tic behavior.
What is a strep carrier?
Some studies have shown that many people can be chronic carriers of strep (about 15-30% of the population depending on the studies). This means that they always test positive for strep even though they may not manifest any symptoms. If your child always tests positive for strep even if their symptoms seem to be atypical they may be a carrier. There is some disagreement about the treatment of suspected carriers, and it should be discussed with your pediatrician.
What about tonsillectomy?
Tonsillectomy (removal of the tonsils) is sometimes necessary for those with recurrent strep infections. Most Ear Nose and Throat doctors require ≥3 episodes in each of three years, ≥5 episodes in each of two years, or ≥7 episodes in one year as an indication for tonsillectomy. If you think your child meets these requirements, then tonsillectomy may be beneficial.
Prevention
Good hand hygiene is always the best way to combat against any infection, especially strep. Be sure to demonstrate and encourage frequent hand-washing to your students this cold season.
The information and content on our website should not be used as a substitute for medical treatment or advice from your doctor.

